New HIV/AIDS treatments 2024
New HIV/AIDS Treatments 2024
HIV, which stands for human immunodeficiency virus, is a virus that attacks the body's immune system, specifically the CD4 cells (T cells), which help the immune system fight off infections. Untreated, HIV reduces the number of CD4 cells in the body, making the person more likely to get other infections or infection-related cancers. Over time, HIV can destroy so many of these cells that the body can't fight off infections and disease. This stage is known as AIDS, or acquired immunodeficiency syndrome, which is the final stage of HIV infection. Not everyone with HIV advances to this stage, and with proper medical care, HIV can be controlled.
When considering treatment options for HIV/AIDS, antiretroviral therapy (ART) is currently the most effective treatment. ART involves taking a combination of HIV medicines (called an HIV treatment regimen) every day. ART is recommended for everyone who has HIV, and it must be taken for life. The goal of HIV treatment is to reduce the viral load to an undetectable level, which keeps the immune system working and prevents illness. It's crucial for individuals to work with their healthcare provider to choose a treatment regimen that fits their needs and to discuss potential side effects and how they can be managed.
Treatment options
| Treatment option | Estimated cost | Efficacy | Eligibility |
|---|---|---|---|
| Antiretroviral Therapy (ART) - Standard Regimen | $2,000 - $5,000 | Highly effective in suppressing viral load | Most adults and children with HIV |
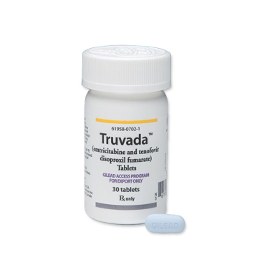
| Truvada (for PrEP) | $1,600 - $2,000 | 92%-99% effective in preventing HIV infection | HIV-negative individuals at high risk for infection |
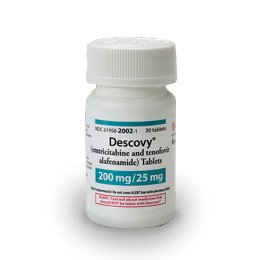
| Descovy (for PrEP) | $1,600 - $2,000 | Similar to Truvada | HIV-negative adults and adolescents at risk for HIV |
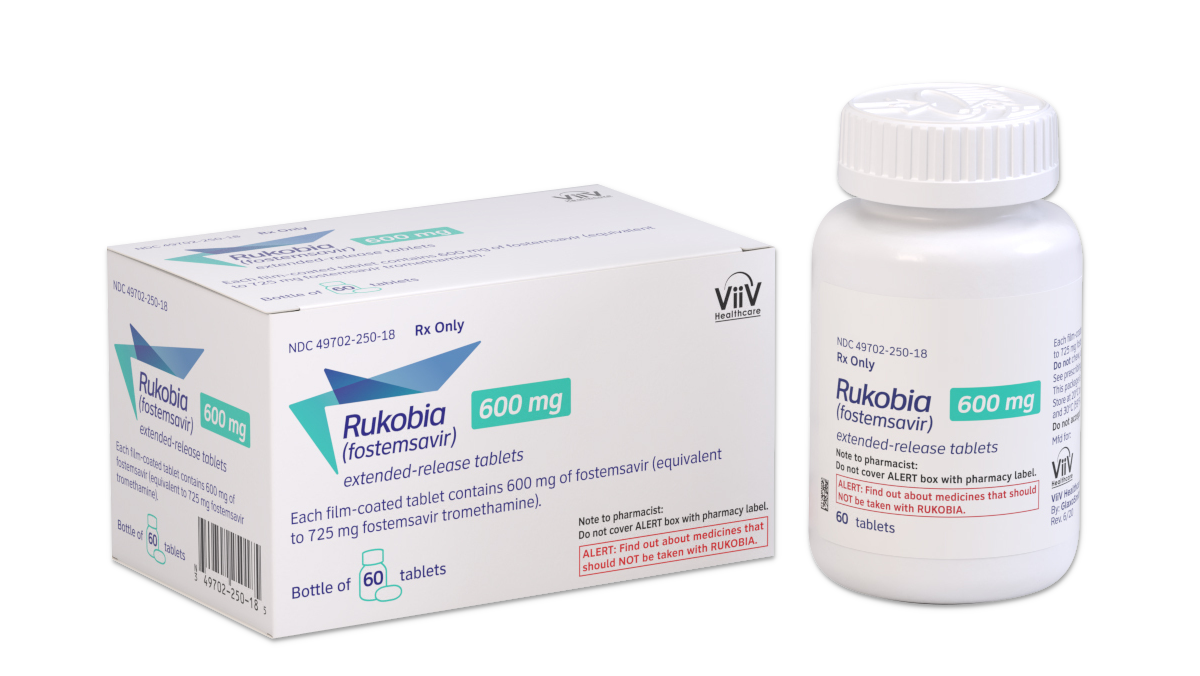
| Rukobia | $5,500 - $6,000 | Effective in heavily treatment-experienced adults | Adults with multidrug-resistant HIV-1 infection |
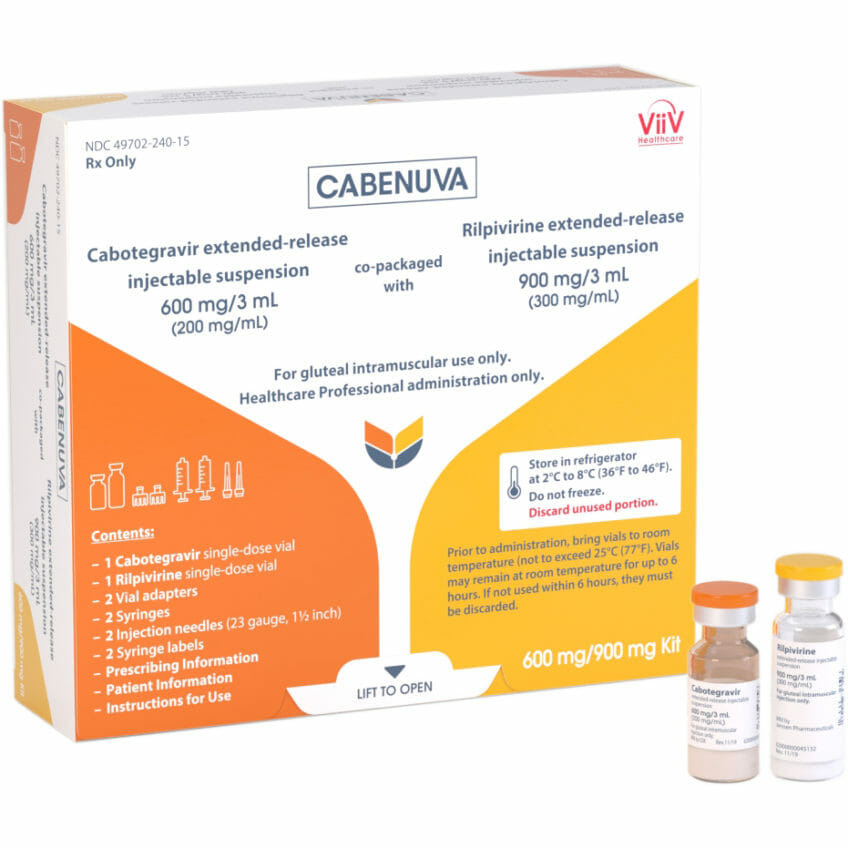
| Cabenuva | $3,700 - $4,500 | Effective in maintaining viral suppression | Adults who are virologically stable and suppressed |
| Vocabria (in combination with Cabenuva) | $3,700 - $4,500 (combined with Cabenuva) | Effective in maintaining viral suppression | Adults on stable antiretroviral regimen |
| Pifeltro | $2,100 - $2,500 | Effective in achieving viral suppression | Adults with no prior antiretroviral treatment history |
| Apretude (injectable PrEP) | $3,000 - $3,500 | 69% more effective than daily oral PrEP | HIV-negative adults and adolescents at risk for HIV |
| Biktarvy | $3,000 - $3,500 | Highly effective in suppressing viral load | Adults and children who weigh at least 25 kg |
| Sunlenca (lenacapavir) | $3,000 - $3,500 | Effective in heavily treatment-experienced adults | Adults with multidrug-resistant HIV-1 infection |
| Experimental Treatments | Variable | Varies by treatment and study phase | Typically participants in clinical trials |
Treatments options in detail
Antiretroviral Therapy (ART)
The cornerstone of HIV/AIDS treatment is antiretroviral therapy (ART), which involves a combination of antiretroviral (ARV) medications. ART works by reducing the amount of HIV in the body, known as the viral load, to undetectable levels. This helps to boost the immune system and prevent the progression of HIV to AIDS. The most common ART regimen combines three or more ARVs from at least two different drug classes to avoid creating drug-resistant strains of HIV.
Nucleoside Reverse Transcriptase Inhibitors (NRTIs)
NRTIs are one of the first classes of ARVs used in ART. They function by blocking the reverse transcriptase enzyme, which HIV uses to replicate its genetic material. Truvada, a combination of emtricitabine and tenofovir disoproxil fumarate, is a popular NRTI medication often used in treatment regimens and as pre-exposure prophylaxis (PrEP) to prevent HIV infection in high-risk individuals. Descovy, which contains emtricitabine and tenofovir alafenamide, is another NRTI that is similar to Truvada but with a different formulation of tenofovir, designed to be gentler on the kidneys and bones.
Integrase Strand Transfer Inhibitors (INSTIs)
INSTIs block the integrase enzyme, which HIV uses to integrate its genetic material into the host cell's DNA. Biktarvy is a single-tablet regimen that combines bictegravir, an INSTI, with emtricitabine and tenofovir alafenamide. It is favored for its high efficacy, safety profile, and ease of use, requiring only one pill per day.
Non-Nucleoside Reverse Transcriptase Inhibitors (NNRTIs)
NNRTIs bind to and inhibit the reverse transcriptase enzyme in a way that is different from NRTIs. Pifeltro (doravirine) is a newer NNRTI that is taken once daily and is known for its high barrier to resistance and lower risk of side effects compared to older NNRTIs.
Protease Inhibitors (PIs)
PIs interfere with the protease enzyme, which HIV uses to cut viral proteins into the proper lengths for creating new virus particles. PIs are often boosted with another medication, such as ritonavir or cobicistat, to increase their effectiveness.
Entry Inhibitors and Fusion Inhibitors
These medications block HIV's entry into host cells. Entry inhibitors bind to proteins on the surface of either the virus or the host cell, preventing the virus from attaching to the host cell. Fusion inhibitors prevent HIV from merging with the host cell membrane, thus blocking entry into the cell.
Long-Acting Injectable ART
Cabenuva is a long-acting injectable ART regimen that includes the integrase inhibitor cabotegravir and the NNRTI rilpivirine. It is administered once monthly or every two months, providing an alternative to daily oral medication. Vocabria is the tablet form of cabotegravir used in combination with oral rilpivirine for a short lead-in period before starting Cabenuva injections.
Monoclonal Antibodies
Monoclonal antibodies are an experimental treatment that is not yet approved by the FDA for HIV. These antibodies are designed to target specific parts of the HIV virus, marking it for destruction by the immune system. Research is ongoing to determine their efficacy and safety in treating HIV/AIDS.
Attachment Inhibitors
Rukobia (fostemsavir) is an attachment inhibitor approved for use in adults with multidrug-resistant HIV who have limited treatment options. It works by blocking the gp120 protein on the surface of HIV, preventing the virus from attaching to and entering CD4 cells.
HIV-1 Capsid Inhibitors
Sunlenca (lenacapavir) is an experimental HIV-1 capsid inhibitor that has shown promise in clinical trials. It works by interfering with multiple stages of the HIV lifecycle, including capsid assembly and disassembly, which are essential for viral replication. Sunlenca is not yet approved by the FDA but represents a potential new class of ARV medication.
Long-Acting PrEP
Apretude (cabotegravir extended-release injectable suspension) is a long-acting form of PrEP approved by the FDA for reducing the risk of sexually acquired HIV-1 infection. It is administered as an injection every two months after an initial loading phase and offers an alternative to daily oral PrEP medications.
Adjunctive Therapies
While ART remains the primary treatment for HIV/AIDS, adjunctive therapies may also be used to address specific complications or comorbidities associated with HIV infection. These can include medications for opportunistic infections, mental health conditions, and other health issues that may arise in individuals living with HIV/AIDS.
Experimental Treatments and Cure Research
Researchers continue to explore new treatment options, including therapeutic vaccines, gene editing technologies like CRISPR, and other novel agents that could potentially eradicate HIV from the body or induce a functional cure where the virus is controlled without the need for ongoing ART. These experimental treatments are still in various stages of research and development and are not widely available outside of clinical trials.
Considerations for Treatment Selection
The selection of an appropriate HIV treatment regimen is based on several factors, including the individual's health status, potential drug-drug interactions, side effect profiles, and the presence of any drug-resistant strains of HIV. Patients should work closely with their healthcare providers to choose the best treatment plan for their specific situation.
Monitoring and Adherence
Regular monitoring of viral load and CD4 counts is crucial to assess the effectiveness of ART and make any necessary adjustments to the treatment regimen. Adherence to ART is essential for maintaining an undetectable viral load and preventing the development of drug resistance. Healthcare providers will work with patients to address any barriers to adherence, which may include side effects, pill fatigue, or other challenges.
Conclusion
The treatment landscape for HIV/AIDS has evolved significantly over the years, offering a range of options that can lead to a near-normal life expectancy for those with access to and adherence to effective ART. Ongoing research continues to expand the arsenal of HIV treatment options, improving the quality of life for those living with the virus and moving closer to the ultimate goal of a cure.
Symptoms
Acute HIV Infection Symptoms
The initial stage of HIV infection is known as acute HIV infection or primary HIV infection. It occurs within 2 to 4 weeks after the virus is contracted. During this phase, individuals may experience a flu-like illness, which is the body's natural response to the infection. Symptoms can include fever, which is the most common symptom, along with a sore throat, swollen lymph nodes, and a rash. Other symptoms can include muscle aches, joint pain, headache, and diarrhea. Some individuals may also experience nausea and vomiting. It is important to note that not everyone will experience symptoms during this stage, and those who do might not recognize them as signs of HIV infection.
Asymptomatic HIV Infection
After the acute stage, HIV may enter a prolonged asymptomatic period. During this time, individuals may not exhibit any symptoms despite the virus continuing to multiply and damage the immune system. This stage can last for several years and without testing, a person may not be aware they are infected. Regular monitoring and testing are crucial during this phase to manage the virus and maintain health.
Symptomatic HIV Infection
As the immune system becomes more compromised, symptoms may begin to emerge. These can include the persistent enlargement of lymph nodes, often one of the first signs of HIV infection. Other symptoms that might appear include weight loss, fever, and diarrhea, which persist for an extended period. As the virus progresses, it can lead to an increased susceptibility to opportunistic infections due to the weakened immune system.
AIDS-Defining Illnesses
When HIV progresses to its most advanced stage, Acquired Immunodeficiency Syndrome (AIDS), individuals can develop a range of more severe symptoms. These symptoms are often associated with the opportunistic infections and cancers that the compromised immune system can no longer fight off. Common opportunistic infections include Pneumocystis pneumonia, a fungal infection that can cause severe illness; Kaposi's sarcoma, a type of cancer that affects the skin and internal organs; and Candidiasis, a fungal infection that can affect the mouth, throat, and esophagus. Other opportunistic infections can include tuberculosis, cytomegalovirus, toxoplasmosis, and cryptococcal meningitis.
Neurological Symptoms
HIV can affect the nervous system, leading to neurological symptoms. This can result in conditions such as HIV-associated dementia or AIDS dementia complex, which can cause cognitive impairments, motor dysfunction, and behavioral changes. Other neurological symptoms may include peripheral neuropathy, which is characterized by numbness, tingling, or pain in the extremities. In some cases, individuals may experience seizures or develop progressive multifocal leukoencephalopathy (PML), a rare brain infection that can be life-threatening.
Gastrointestinal Symptoms
Gastrointestinal symptoms are common in individuals with HIV/AIDS. These can include chronic diarrhea, which is often caused by opportunistic infections or the HIV virus itself. Other symptoms include nausea, vomiting, and abdominal pain. These gastrointestinal issues can contribute to significant weight loss and malnutrition, often referred to as "wasting syndrome."
Respiratory Symptoms
Respiratory symptoms can also be prevalent in those with HIV/AIDS, particularly as the disease progresses. Shortness of breath, coughing, and difficulty breathing can be signs of opportunistic lung infections such as Pneumocystis pneumonia or tuberculosis. These symptoms should be taken seriously as they can indicate life-threatening conditions requiring immediate medical attention.
Integumentary Symptoms (Skin and Mucous Membrane)
Skin rashes and lesions are common symptoms of HIV infection. The appearance of these skin issues can vary widely, from mild to severe. They are often the result of opportunistic infections or as a direct result of the virus itself. Herpes zoster (shingles) and herpes simplex viruses can cause painful skin sores, while oral hairy leukoplakia can cause white patches on the tongue or inside the mouth. Additionally, individuals with advanced HIV/AIDS may develop Kaposi's sarcoma, which appears as dark or purple lesions on the skin or mucous membranes.
Other Symptoms
There are numerous other symptoms that can be associated with HIV/AIDS. Night sweats, persistent fatigue, and unexplained bleeding or bruising can occur as the immune system deteriorates. Women with HIV may experience changes in their menstrual cycle, including irregular periods or even the cessation of periods. Individuals may also suffer from recurrent or severe colds and other infections due to the weakened immune system.
Importance of Testing and Monitoring
It is crucial for individuals who may have been exposed to HIV to undergo testing, as many of the symptoms of HIV can be nonspecific and similar to those of other illnesses. Early detection and treatment with antiretroviral therapy can help manage symptoms, reduce the progression of the virus, and improve quality of life. Regular monitoring by healthcare professionals is essential for individuals living with HIV/AIDS to manage the disease and its symptoms effectively.
Cure
Current Status of HIV/AIDS Cure
As of the current medical consensus, there is no definitive cure for HIV/AIDS. The human immunodeficiency virus (HIV) is a complex retrovirus that attacks the immune system, specifically the CD4 T cells, which are crucial for fighting infections. Once the immune system is compromised, Acquired Immunodeficiency Syndrome (AIDS) can develop, leading to a host of life-threatening infections and cancers.
Antiretroviral Therapy (ART)
The primary treatment for HIV is antiretroviral therapy (ART), which involves a combination of medicines that work to suppress the virus to undetectable levels in the blood. ART doesn't cure HIV but helps individuals maintain a high quality of life by preventing the progression of the virus to AIDS. When taken consistently, ART can reduce the viral load to such an extent that it is not transmissible to others, a concept known as 'undetectable = untransmittable' (U=U).
Attempts at Eradicating HIV
There have been numerous attempts to eradicate HIV from the body, including strategies like 'shock and kill' where dormant HIV is activated and then destroyed, and 'block and lock' which aims to keep the virus permanently inactive. However, these strategies have not yet led to a cure. The main challenge in curing HIV is the presence of viral reservoirs – cells where HIV remains hidden and integrated into the host DNA, unaffected by the immune response or current treatments.
Notable Cases of Remission
There have been rare instances of individuals achieving remission from HIV. The most famous cases are the 'Berlin patient' and the 'London patient,' both of whom underwent stem cell transplants from donors with a rare genetic mutation (CCR5-delta 32) that confers resistance to HIV. These cases have been extensively studied and have provided hope and direction for research into a potential cure, but stem cell transplantation is a high-risk procedure not suitable as a general treatment for HIV due to its complexity and potential for severe complications.
Gene Therapy and Editing
Gene therapy and gene editing are emerging fields that offer potential avenues for an HIV cure. By using techniques such as CRISPR-Cas9, researchers are exploring ways to edit the CCR5 receptor on human cells, which is a critical entry point for most strains of HIV. While promising, these approaches are still in the experimental stages and face significant ethical and technical challenges before they can be considered viable treatments.
Vaccine Development
Efforts to develop a preventive HIV vaccine have been ongoing for decades, but no effective vaccine is available yet. A vaccine would not cure HIV but could prevent the infection from occurring. Several vaccine candidates have reached clinical trials, but none have provided sufficient protection to be approved for general use. Vaccine research continues to be a critical area of study in the fight against HIV/AIDS.
Functional Cure
A functional cure, where the virus is controlled without the need for ongoing therapy, is considered a more achievable goal in the near term than a sterilizing cure, which would completely eradicate the virus. A functional cure would allow individuals to maintain a healthy immune system and prevent the transmission of the virus without daily medication. Research in this area includes therapeutic vaccines, immune modulators, and other strategies to enhance the body's natural ability to control the virus.
Pre-Exposure Prophylaxis (PrEP)
While not a cure, pre-exposure prophylaxis (PrEP) is a preventive strategy that has significantly impacted the management of HIV. PrEP involves taking antiretroviral medication regularly by individuals who do not have HIV but are at high risk of contracting it. PrEP has been shown to reduce the risk of HIV infection by up to 99% when taken consistently.
Conclusion
In conclusion, while there is currently no cure for HIV/AIDS, there is effective treatment available that can manage the virus and prevent its progression to AIDS. Research into a cure continues to be a field of intense study, with advances in gene therapy, immune-based therapies, and other innovative approaches offering hope for the future. Until a cure is found, prevention strategies like PrEP, along with ART for those living with HIV, remain the cornerstones of HIV management.
Access HIV/AIDS medicines today
If HIV/AIDS medicines are not approved or available in your country (e.g. due to supply issues), you can access them via Everyone.org.
How Everyone.org works

Make an enquiry
Choose the medicine you want to access, answer a couple of questions, and upload your prescription to speed things up. We’ll get back to you within 24 hours.


Make an enquiry
Choose the medicine you want to access, answer a couple of questions, and upload your prescription to speed things up. We’ll get back to you within 24 hours.


Breeze through the paperwork
We'll guide you through the required documents for importing unapproved medicine, ensuring you have all the necessary information.


Get a personalized quote
We’ll prepare a quote for you, including medicine costs and any shipping, administrative, or import fees that may apply.


Receive your medicine
Accept the quote and we’ll handle the rest - sourcing and safely delivering your medicine.

Some text on this page has been automatically generated. Speak to your physician before you start a new treatment or medication.
Let's talk
If you have any questions, call us or send us a message through WhatsApp or email:
Contact us